Understanding Anxiety, Depression, and Brain Fog During the Menopausal Transition
- Gurprit Ganda

- Feb 16
- 6 min read

When Your Mind and Body Are Changing at the Same Time
You have always been able to cope. You have managed work, family, and daily life without missing a beat. But lately, something feels different. You cannot concentrate like you used to. You feel anxious for no clear reason. You snap at your partner and children over small things. You lie awake at 3am with a racing mind. And some days, a fog settles over your brain that makes even simple tasks feel exhausting.
If you are a woman between the ages of 40 and 55, these experiences may not be "just stress." They may be symptoms of perimenopause — the transitional phase before menopause when your hormones begin to fluctuate and decline. And the mental health impact can be just as significant as the physical symptoms.
Research published in the Journal of Mid-life Health in 2025 identifies perimenopause as a "window of vulnerability" for new-onset anxiety and depression. Women are 2 to 5 times more likely to develop a mood disorder during perimenopause compared to before it begins (McElhany et al., 2024). Yet many women — and their doctors — do not connect these psychological changes to hormonal shifts.
What Is Perimenopause (Menipausal Transition) and How Does It Affect Your Brain?
Perimenopause is the transition period leading up to menopause. It typically begins in a woman's mid-40s but can start earlier. During this time, your ovaries gradually produce less estrogen and progesterone. This process can take anywhere from a few months to over a decade.
What many women do not realise is that estrogen is not just a reproductive hormone. It is a powerful neuroactive steroid that directly affects your brain. Estrogen modulates serotonin (your mood-regulating neurotransmitter), dopamine (motivation and pleasure), GABA (your brain's natural calming chemical), and norepinephrine (alertness and focus). When estrogen levels fluctuate unpredictably during perimenopause, these neurotransmitter systems become unstable (PMC, 2025). This is why you may feel anxious one day, flat the next, and unable to think clearly the day after.

A 2025 integrative review published in the World Journal of Psychiatry explained that estrogen decline disrupts the hypothalamic-pituitary-adrenal (HPA) axis, increases inflammatory processes, and reduces neurotrophic factor expression — all of which contribute to mood disturbance and cognitive difficulties.
Symptoms That Look Like Anxiety and Depression — But Are Hormonal
Perimenopausal mental health symptoms often overlap with anxiety and depression, making them easy to misdiagnose. Research from the SWAN (Study of Women's Health Across the Nation) study found that approximately 51% of women reported irritability, nervousness, or frequent mood changes during the menopausal transition.
Common psychological symptoms include: persistent anxiety or a sense of dread without clear cause; irritability and emotional reactivity that feels out of proportion; difficulty concentrating or "brain fog" including memory lapses; low mood, loss of interest, or feelings of emptiness; sleep disruption including insomnia and night waking; loss of confidence or sense of identity; and overwhelming fatigue that rest does not resolve.

The challenge is that these symptoms often develop gradually. Women may attribute them to work stress, relationship difficulties, or "just getting older." A 2025 study in BMC Women's Health found that women with sleep problems during perimenopause were approximately three times more likely to report anxiety symptoms than those without sleep problems (Jiang et al., 2025).
When "Brain Fog" Is More Than Forgetfulness
Cognitive changes during perimenopause are real and well-documented. These changes often mirror symptoms seen in ADHD, including declines in verbal memory and executive function (Deshpande & Rao, 2025). Estrogen plays a critical role in the prefrontal cortex (planning and decision-making), hippocampus (memory and learning), and amygdala (emotional regulation).
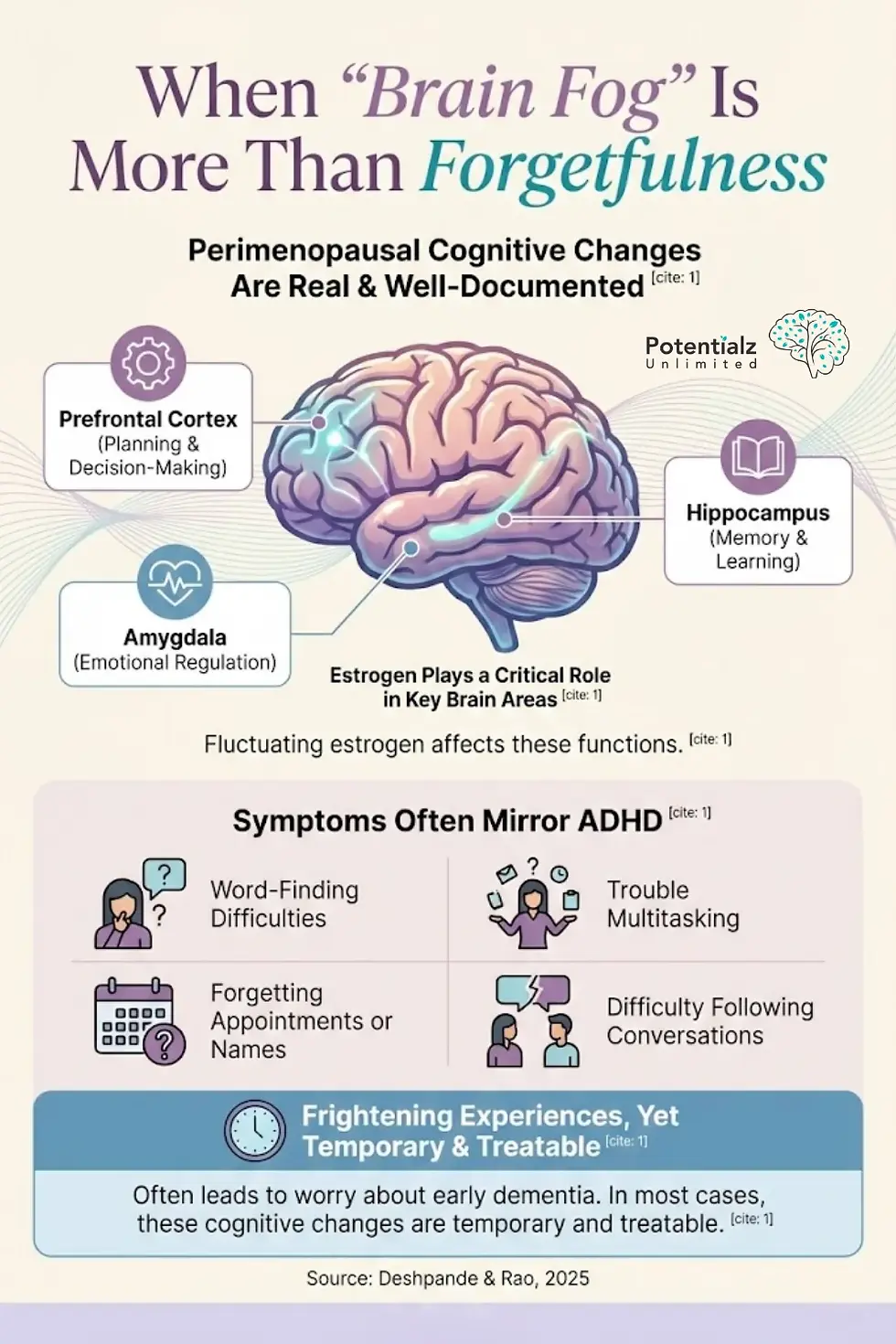
When estrogen fluctuates, women may experience word-finding difficulties, trouble multitasking, forgetting appointments or names, and difficulty following conversations. These experiences can be frightening and often lead women to worry about early dementia. In most cases, perimenopausal cognitive changes are temporary and treatable.
How CBT and Psychological Therapy Help During Menopausal Transition Related Anxiety
Evidence-based psychological therapy is one of the most effective treatments for perimenopausal mental health symptoms (such as menopausal transition related anxiety) . A 2025 systematic review and meta-analysis of 30 studies (pooled sample of 3,501 participants) found that both CBT and Mindfulness-Based Interventions significantly improved anxiety and depressive symptoms in menopausal women. CBT demonstrated significant effects in reducing anxiety (d = -0.22) and depression (d = -0.33), while Mindfulness-Based Interventions showed medium effect sizes for anxiety (d = -0.56) (Spector et al., 2025).
At Potentialz Unlimited in Bella Vista, our psychologists provides CBT specifically adapted for perimenopause. This includes helping you identify and challenge unhelpful thought patterns about menopausal symptoms; developing practical coping strategies for anxiety and mood changes; addressing sleep disruption using CBT for insomnia (CBT-I); building mindfulness skills for managing hot flashes and emotional reactivity; and supporting you through the identity shifts that often accompany midlife.

Importantly, CBT for perimenopause works alongside medical treatment. The North American Menopause Society recommends that proven therapeutic options for depression — including psychotherapy — are front-line treatments for perimenopausal depression (Maki et al., 2019).
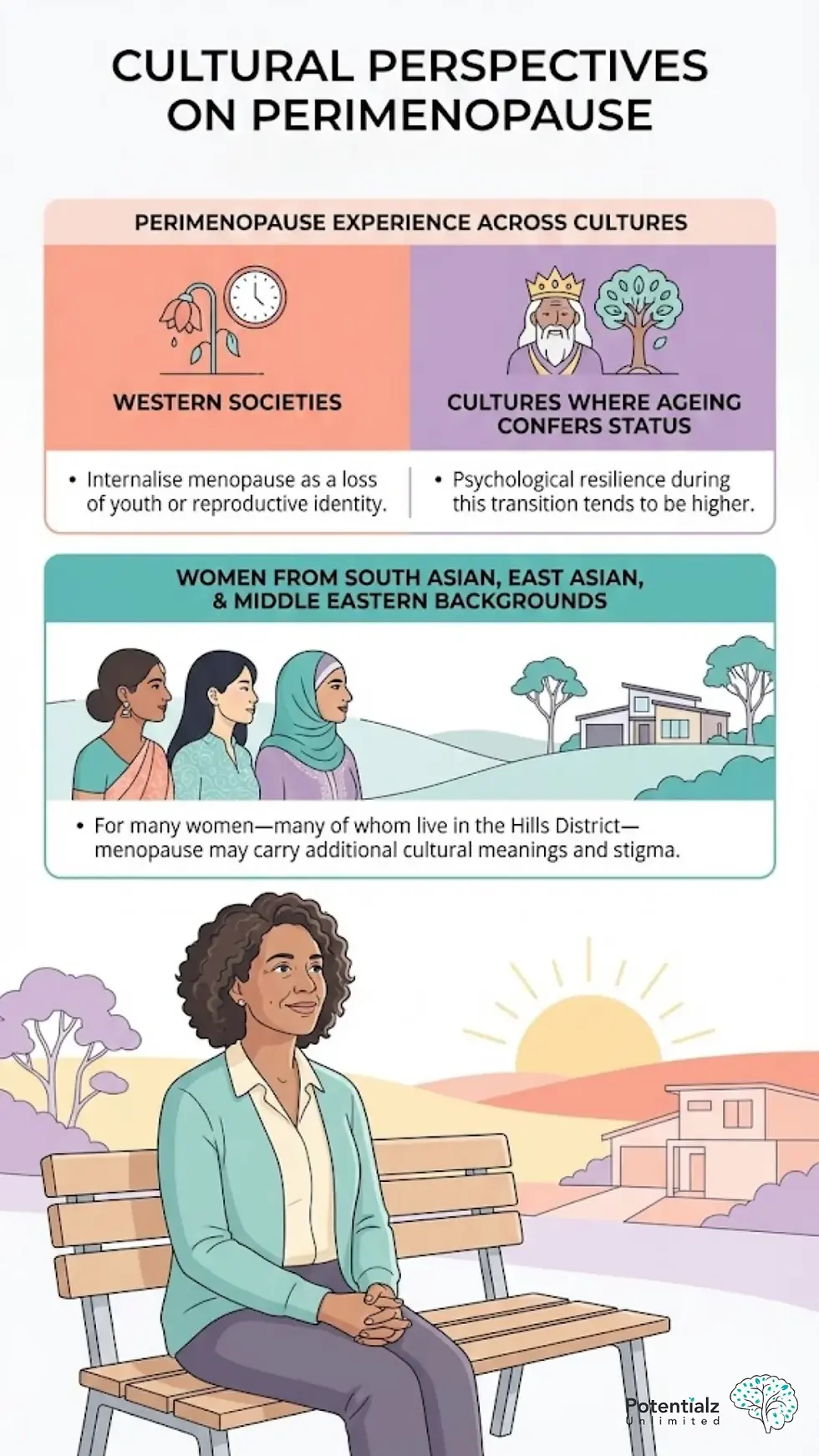
Cultural Considerations for Multicultural Women in the Hills District
Perimenopause is experienced differently across cultures. Research shows that women in Western societies may internalise menopause as a loss of youth or reproductive identity, whereas in cultures where ageing confers status, psychological resilience during this transition tends to be higher (Deshpande & Rao, 2025). For women from South Asian, East Asian, and Middle Eastern backgrounds — many of whom live in the Hills District — menopause may carry additional cultural meanings and stigma.
At Potentialz Unlimited, we provide culturally responsive care that respects your background and values. Dr Ganda brings over 22 years of experience working with multicultural families and understands the unique challenges faced by women navigating perimenopause across cultural contexts.
When to See a Psychologist for Perimenopause Anxiety and Depression in Bella Vista
Consider seeking psychological support if your mood changes are interfering with daily life, work, or relationships; if you feel anxious or depressed more days than not; if brain fog is affecting your ability to function; if sleep problems persist despite good sleep hygiene; if you feel you have lost your sense of self or purpose; or if you are struggling with the emotional weight of midlife changes.
Related Blog Posts
The Complex Dance of Anxiety and Sleep Disturbances
References (APA 7th Edition)
Deshpande, N., & Rao, T. S. S. (2025). Psychological changes at menopause: Anxiety, mood swings, and sexual health in the biopsychosocial context. Journal of Psychosexual Health, 7(1), 1–8. https://doi.org/10.1177/26318318251324577
Jiang, M., Chen, L., Zheng, X., & Feng, Y. (2025). Latent profile analysis of symptoms of depression and anxiety among perimenopausal women and their predictors. Frontiers in Psychiatry, 16, 1572570. https://doi.org/10.3389/fpsyt.2025.1572570
Maki, P. M., Kornstein, S. G., et. al. (2019). Guidelines for the Evaluation and Treatment of Perimenopausal Depression: Summary and Recommendations. Journal of women's health (2002), 28(2), 117–134. https://doi.org/10.1089/jwh.2018.27099.mensocrec
McElhany, K., et al. (2024). Protective and harmful social and psychological factors associated with mood and anxiety disorders in perimenopausal women. Maturitas, 190, 108118. https://doi.org/10.1016/j.maturitas.2024.108118
PMC. (2025). From physiology to psychology: An integrative review of menopausal syndrome. World Journal of Psychiatry, 15(3). https://pmc.ncbi.nlm.nih.gov/articles/PMC12635657/
Spector, A., Li, Z., He, L., Badawy, Y., & Desai, R. (2024). The effectiveness of psychosocial interventions on non-physiological symptoms of menopause: A systematic review and meta-analysis. Journal of Affective Disorders, 352, 460–472. https://doi.org/10.1016/j.jad.2024.02.048
Zhang, Y., et al. (2025). Global, regional, and national burden of anxiety disorders during the perimenopause (1990-2021) and projections to 2035. BMC Women's Health, 25(1), 11. https://doi.org/10.1186/s12905-025-03547-z




Comments